By Jo Adaway
Consultant Clinical Scientist, Biochemistry
December 2023
The workload for 25(OH) Vitamin D has increased year on year, from 73,394 in 2014 to 89,040 in 2022. This workload is unsustainable as our staff and analysers are struggling to keep up with the demand for the test. The issue is not limited to our Trust, Biochemistry departments across Greater Manchester have also noted a massive increase in Vitamin D workload, and work has been started within the Greater Manchester Pathology Network (GMPN) to look at how we ensure all the Vitamin D tests we analyse are clinically appropriate.
NICE has published guidance on Vitamin D deficiency in adults and this was used as the basis for recommendations for Vitamin D testing in adults which are being adopted across GMPN. Recent studies such at the VITAL study suggest that the NICE guidance is appropriate, as reported in the October 2022 issue of Lab Report.
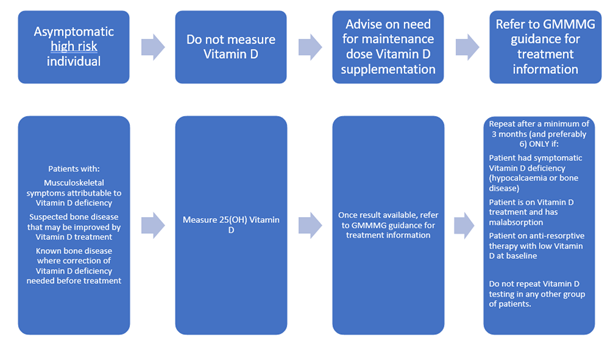
Asymptomatic individuals at high risk of Vitamin D deficiency should be treated without measurement of Vitamin D and should be advised on the need for maintenance dose Vitamin D supplementation. Advice on supplementation can be found in GMMMG guidance. Vitamin D should only be measured in patients with:
- Musculoskeletal symptoms that may be attributable to Vitamin D deficiency
- Suspected bone disease such as osteomalacia or osteoporosis that may be improved with Vitamin D treatment
- Known bone disease such as osteoporosis or Paget’s disease, where correction of Vitamin D deficiency is needed prior to specific treatment (for example antiresorptive agents, such as alendronate, zoledronate, denosumab, or teriparitide)
In addition, repeat Vitamin D measurement is not recommended in the majority of patients. Repeat measurement should only be considered in patients:
- Who had symptomatic Vitamin D deficiency (e.g. hypocalcaemia or bone disease)
- Who have malabsorption and are taking Vitamin D
- Who are on oral anti-resorptive agents and whose Vitamin D levels were low at baseline
Repeat testing should not be done within three months of the initial test, and preferably not within six months.
This guidance is highlighted here:
In order to implement this guidance we are planning to put a series of questions in ICE to determine the appropriateness of the request. If the answers indicate that the request does not meet the NICE criteria for testing, the system will not allow the request to be made. You will also be asked if a request has been made in the past three months, and you will not be allowed to make the request if the answer to this question is yes. Once the sample is received in the lab and booked in, the lab IT system will check for a previous result within the past three months, and, if one is found, a report will automatically be generated stating that repeat testing within three months is not recommended, and the sample will not be analysed for Vitamin D.
If you are trying to request Vitamin D on a patient who does not meet the criteria, but you feel clinically requires the test, you can call the Duty Biochemist 9am-5pm, Monday to Friday, to discuss this, and they will be able to facilitate the requesting if it is required. The Duty Biochemist for Central and North GPs can be reached on 701 8891, South and Trafford GPs should call 291 2136.
If you have any comments or questions about the proposed implementation of Vitamin D demand optimisation, please email jo.adaway@mft.nhs.uk