If you have been referred for IVF treatment at Saint Mary’s, we ask both partners to watch this video which describes the process, success rates and risks of fertility treatment. We want to ensure that all our patients fully understand what is involved in having fertility treatment. Please make a note of any questions that you may have after watching the video. The doctor or nurse at your consultation will be able to answer these questions. Confirmation of your/your partner’s consent will be undertaken on our fertility platform.
What is IVF?
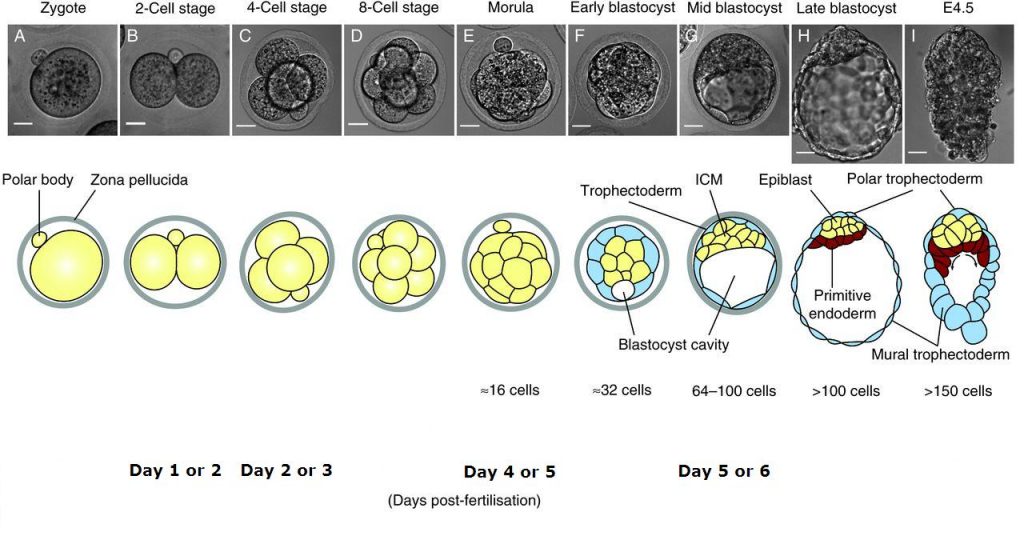
IVF stands for ‘In vitro fertilisation’. This is a type of fertility treatment in which eggs are fertilised with sperm in the laboratory to create embryos. These embryos are then transferred to the womb with the aim of achieving a pregnancy and birth.
This treatment may be recommended for couples with infertility due to a number of reasons. In some cases, other treatments will have been tried first, while in other cases there is no other treatment except IVF.
There are two methods of fertilisation of eggs in the laboratory. In ‘standard IVF’ the eggs and sperm are mixed together and allowed to fertilise naturally. This is advised where there is no significant concern about sperm numbers or quality. However, in couples facing challenges related to sperm health or function, an alternative method of fertilisation is used, called ‘ICSI’. This stands for Intra-Cytoplasmic Sperm Injection. In this technique, individual sperm are selected and injected into individual mature eggs by the scientist.
Couples are notified of the number of fertilised eggs the morning after egg collection. Usually all fertilised eggs (also called embryos) are cultured in the incubator for possible embryo transfer on day 2, day 3 or day 5.
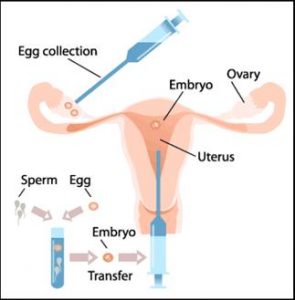
What does the treatment involve?
We currently use two IVF/ICSI cycle types:
- Long down-regulation protocol: uses GnRH Agonist and Gonadotrophin injections
- Antagonist protocol: uses GnRH Antagonist and Gonadotrophin injections
The team will decide which protocol best suits your individual circumstances. The protocol for each cycle is tailor-made to the individual based on various parameters, including hormone test results, previous cycle response and associated medical history. This will be discussed with you at your clinic appointment.
You will be booked into a nurse appointment who will carry out your pre-op and answer any questions you have about your treatment.
Each treatment cycle lasts approximately 6-8 weeks.
Whichever protocol you are on, there are several stages that are common to both:
 In this section
In this section