Our centre
Manchester Centre for Neonatal Surgery (MCNS) is one of the largest for neonatal surgery in the UK and carries out approximately 200 operations each year.
We care for babies who need operations because they are born prematurely or with birth defects.
MCNS is run by teams from Royal Manchester Children’s Hospital and St Mary’s Hospital.
Care in one place
At Manchester our maternity suite, neonatal intensive care unit (NICU), and operating theatres are close together in the same building.
This co-location helps babies and their parents towards better outcomes during the first few days.
Babies born with us do not have to travel or transfer to another hospital. This means babies who may be fragile are disturbed less.
If a baby in our care needs urgent surgery after being born, they are seen very quickly by a specialist surgeon. Also the operating theatres are close so the operation can take place straight away. This saves time which can be critical for some babies.
The wellbeing of mothers and babies is better when they spend more time together. By not having to travel, mothers and babies spend more time together, which will help them bond.
Care for life from the beginning
At our site, we care for people and families for life in one place. Our services start with family planning and fertility treatment, through pregnancy (obstetrics), babies (neonatal), children (paediatrics), and into adulthood.
This means we can reassure our patients by giving them care that is easy to access and stable as they grow up.
Specialist care
Our doctors and nurses specialise in treating rare conditions and because lots of babies are treated by us, our team has a high level of expertise.
MCNS is one of a few UK centres to have dedicated teams of surgeons for the following:
- Oesophageal atresia (OA/TOF)
- Anorectal malformations
- Hirschsprung’s disease
- Sacrococcygeal teratoma
We’ve plenty of information on conditions we treat, and our specialist clinics.
Our team
Our team have different specialisms and expertise, but work closely together to care for newborn babies who need operations. They review each baby’s care every day to make sure every baby is getting the best care.
Each week the team meet up in a Multi-Disciplinary Team (MDT) meeting to discuss the care of all babies. This team working together is essential to ensure all babies get excellent care.
The specialists who attend the MDT meeting include; consultant neonatal surgeons, consultant neonatologists, consultant anaesthetists, neonatal nurses and dieticians.
Patient stories
April and Evie’s story
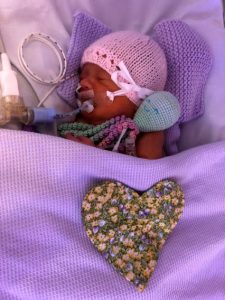
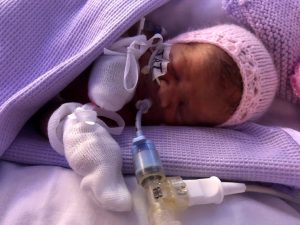
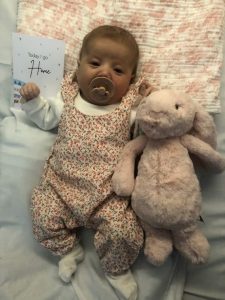
April and Evie were both born with the rare birth defect; Oesophageal Atresia (OA) with Tracheo-Oesophageal Fistula (TOF), which affects approximately 1 in 4,000 newborns. Within hours of being born, April and Evie underwent life-saving surgery at RMCH.
Harry’s story
At his — week scan, Harry was found to have a large tumour at the base of his spine called a sacrococcygeal teratoma. This condition is rare, affecting 1 in every 40,000 babies. At two hours old, Harry was taken into theatre to have a 9 hour operation to remove the tumour.
Koa’s story
Koa was born with a condition called gastroschisis, which meant his bowels had grown outside of his body near the belly button while in the womb. Within four hours of birth Koa accessed specialist theatres and surgeons for his surgery, and went home after 3-4 weeks in hospital.

Consultants
- Professor Ngozi Edi-Osagie - Consultant Neonatologist and National Clinical Director for Neonatal Care
- Dr Arin Mukherjee - Consultant Neonatologist, Honorary Senior Lecturer at Manchester University
- Dr Michelle Parr - Clinical Lead, Consultant Neonatologist and Honorary Lecturer at Salford University
- Dr Ranganath Ranganna - RCPCH Tutor, Deputy Regional Lead for Paediatrics and Consultant Neonatologist
- Dr Kristin Tanney - Consultant Neonatologist, Clinical Director NICU, Deputy Associate Chief Medical Officer