This section provides information about what you can expect when the time comes to give birth to your baby.
Preparing for the Birth of Your Baby
While it’s nearly impossible to plan for every aspect of your labour and birth, you will probably appreciate feeling prepared. Here are a few things to think through in advance of your birth:
- Create your birth plan, so that you and your midwife/obstetrician are on the same page as to how you’d ideally like your baby to be born. For ideas about what to include in your birth plan, you may find this website useful.
- Pack your hospital bag. This NHS website contains useful information about what you’ll probably want to pack.
- Have a look at a few common labour positions or attend one of the many parent education workshops available.
- Read up on feeding basics. We recommend your baby feeds as soon after birth as is possible. Regardless of your feeding choice, feeding your baby in skin-skin is most beneficial for mum and baby.
- Know the signs of labour so you’ll be aware of what to expect when you contact our maternity triage.
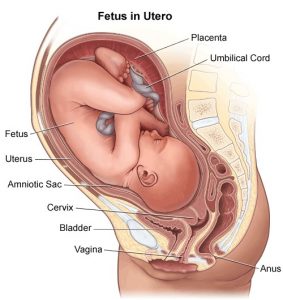 Signs and Stages of Labour
Signs and Stages of Labour
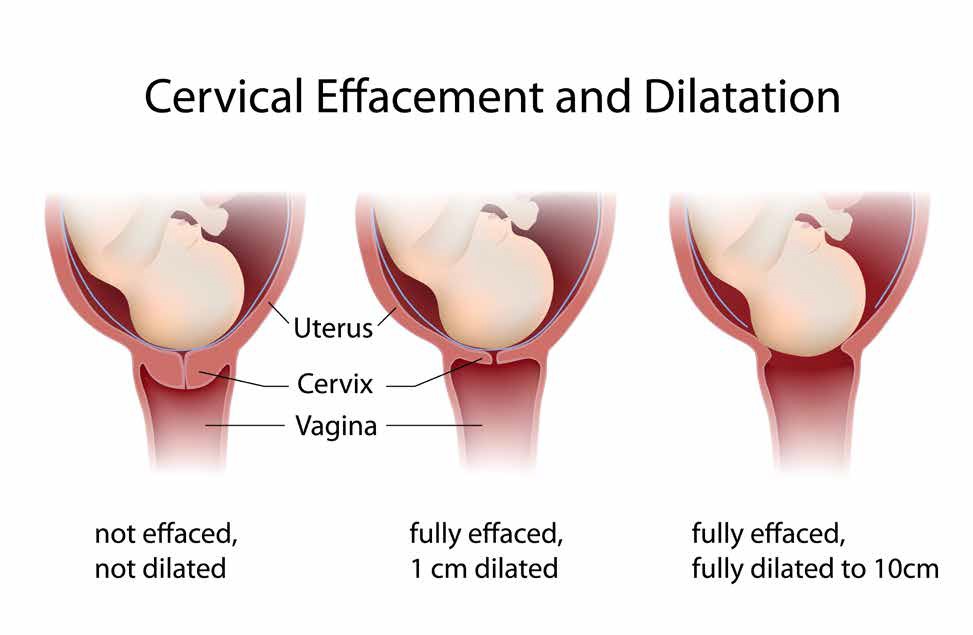
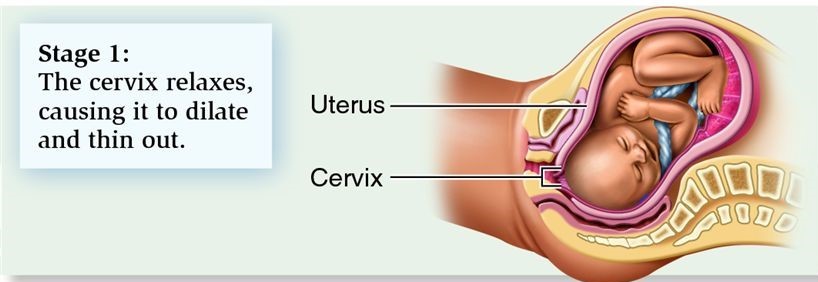
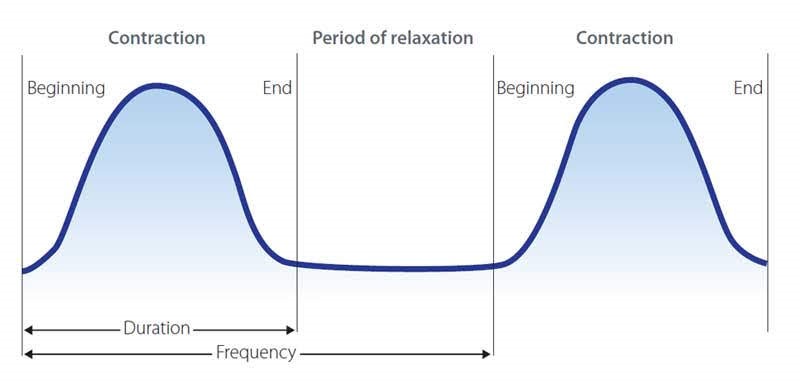
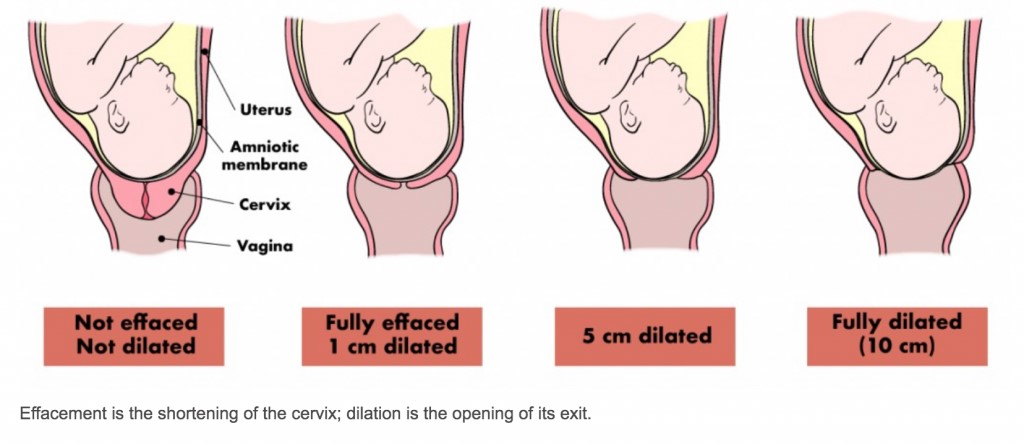
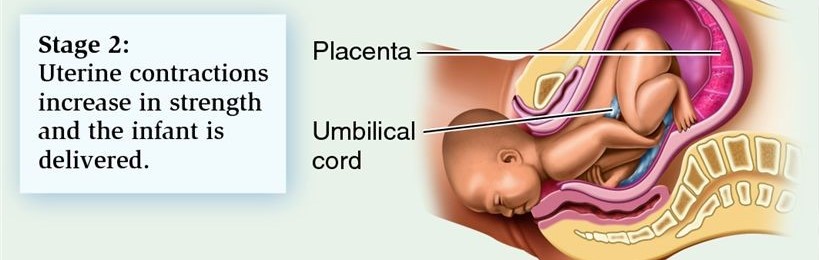
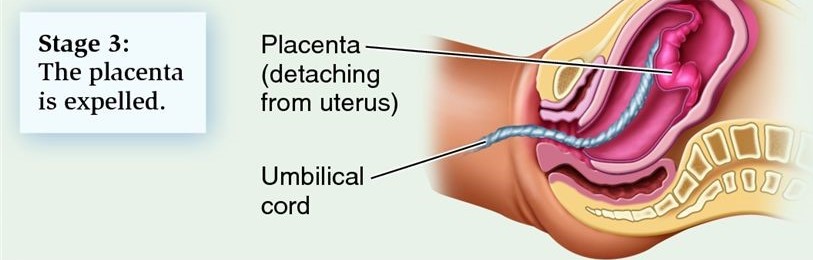
Labour is a gradual process, which involves the womb contracting. This causes the neck of your womb to open and eventually leads to the birth of your baby. Every labour is different and its pattern and progress can be difficult to predict. Here at Saint Mary’s, we are aware that this is a very special and unique time for you. We hope to support you as much as you need through this process. In this section we will describe labour so that you know what to expect. More information is available from your midwife and also parent education classes.
Monitoring your Baby’s Wellbeing in Labour
When you are in established labour, the midwife will want to closely monitor the wellbeing of your baby. This involves monitoring the baby’s heart rate either intermittently or continuously. In an uncomplicated pregnancy, the midwife would recommend intermittently monitoring your baby’s heart rate in labour. If the midwife or doctor have identified any reasons in your pregnancy or labour, that would mean that they recommend continuous monitoring, they will discuss this with you at the start of your labour.
Caesarean Section and Assisted Vaginal Birth
Caesarean Section
A caesarean is usually a planned event and is known as ‘elective’ surgery, which means you are choosing to have it after discussing the reasons with your doctor, midwife or another member of the maternity team. There are several reasons why your doctor may recommend an elective caesarean section- they will discuss the benefits and risks with you so that you can make an informed decision.
Occasionally an emergency caesarean needs to be performed. Reasons for this include concerns about the health of you or your baby or going into labour before a planned caesarean section. More information about caesarean sections.
Assisted Vaginal Birth
Assisted vaginal birth refers to either a vaccum delivery or a forceps delivery. Your doctor and midwife may recommend an operative vaginal delivery if there are concerns about the health of your baby, you have a health condition that means that it is not recommend that you push for a long period of time or your baby is in a position that requires help to deliver their head. Your midwife and doctor will discuss the risks and benefits of an assisted vaginal birth if this is recommended for you. For more information, please see the following link: Assisted Vaginal Birth
Visit here for information on Birth Options After Previous Caesarean Birth
You can also discuss both caesarean sections and assisted vaginal births with your midwife, doctor or in your parent education classes.
The Role of Your Birth Partner
Your birth partner is there to support you throughout the birth of your baby. Your birth partner could be anyone who you feel comfortable with, e.g. your partner, your mum, your friend. Your birth partner should take an active role in supporting you.
Their role may include:
- Making sure that you are well hydrated
- Keeping your birthing environment nice and calm, this may include playing music that you have chosen
- Rubbing your back and shoulders during a contraction, if you find that this gives you some relief
- Positive encouragement
More hints and tips for your birth partner.
For visiting and the number of birth partners allowed, please follow the latest Saint Mary’s advice.
 After the Birth of Your Baby
After the Birth of Your Baby
As long as you and your baby are both well after the birth, you’ll be able to hold your baby straight away. We recommend that your baby is placed straight into skin-skin with you, wherever your baby has been born. Being next to your skin is great at regulating your baby’s heartrate, breathing rate, temperature and gets feeding off to the best start- whatever your feeding choice. Your midwife will discuss skin to skin with you as a part of your birth plan. It is recommended that you have at least an hour of skin to skin with your baby after the birth.
After a vaginal birth, your midwife or doctors will examine your perineum- the skin and muscle between your vagina and your anus- to see whether or not you will require stitches. Normally, these stitches are done in the room where you have birthed your baby, using local anesthetic. If the midwife or doctor feels like better lighting is needed, you need more pain relief or the tear is complex, they may suggest that you are transferred to theatre. The midwife or doctor will discuss caring for your perineum after the birth. You can read more about this here: Episiotomy
Your midwife will recommend Vitamin K for your baby. This is usually given as an injection into your baby’s thigh but can be given orally if you choose. If given orally, your baby may need further doses. Click here for more information about Vitamin K.
If you and your baby are well after the birth, you may be able to go home from the Manchester Birth Centre or Delivery Unit. Your midwife will let you know if they think that this is appropriate for you and your baby. If you or your baby require further monitoring, you need additional feeding support or you do not feel ready to go home so soon, you will be transferred to one of our postnatal wards for ongoing care and support.
 In this section
In this section